By Seraine Page
After the tests, the referrals, the long waits, and the hard conversations with doctors, many parents find themselves asking the same question:
How do I talk to my child about a medical diagnosis?
For parents of medically fragile children, that question often comes while they are still trying to process the diagnosis themselves.
That may include:
- fearing what comes next
- grieving the future they imagined
- wondering how to answer hard questions from their child

One of the most difficult parts is often trying to explain a life-altering diagnosis to a child who wants to laugh, play, and just be a kid.
Perhaps one of the hardest parts for children is that serious medical realities can disrupt the way kids naturally process what they’re going through, according to Micah Clark, licensed professional counselor, On Angels’ Wings board member, and Advanced Certified Grief Recovery Method Specialist.
“With a life-altering diagnosis, children are not going to understand why they can’t just be a kid,” he says. “I think what makes this so hard on the kid is that the one way for the kid to process grief is through play.”
That insight is important for parents who may be trying to sit their child down for a serious conversation, only to find the child resisting, shutting down, or changing the subject.
Below, you’ll find insights from mental health professionals and parents who have lived it for the best ways to talk to your child about a medical diagnosis — with honesty and compassion.
Why Honest Conversations Matter So Much
Children are perceptive. Even very young children can tell when something is wrong, when routines are changing, or when the adults around them are carrying fear.
According to Kristin Christopher, a Florida-based parent and child therapist, the way these conversations are approached can significantly shape how a child understands their diagnosis, processes fear, and builds resilience over time.
“When parents try to minimize what’s happening, it often increases anxiety — for the parent and the child,” says Christopher, who is the founder of Sea Hope Counseling in Saint Augustine, Florida.
When children lack clear information, they often fill in the blanks themselves. And what they imagine may feel far scarier than the truth.
Honesty helps a child feel:
- Included instead of shut out
- Trusted instead of dismissed
- More confident asking questions
That does not mean telling them everything at once. It means giving them truthful information in a way they can actually absorb.
That’s when it’s helpful to remember to start with honesty, not perfection.
Many parents delay these conversations because they are afraid of saying the wrong thing. But your child does not need a flawless speech. They need a parent who is present, grounded, and willing to speak truth gently.
“It’s important for children because they feel trusted [when you’re honest with them],” she says. “You’re planting the seeds of confidence.”
What Honest Communication May Sound Like
The hardest part of having those open communication lines with your child is getting the conversation started.
Kids going through treatment can feel a range of emotions — from numbness to anger and everything in between – and it will show up in many ways, sometimes without them realizing what’s even going on inside.
There’s no single right way to create space for feelings.
Also, not every approach will work every time. What’s most important is that your child understands big feelings are safe to feel and talk about, but the way they respond to those feelings may need redirection. Remember to invite conversation rather than shut it down.
Options to consider:
- Scheduled daily check-ins
- Organic, in-the-moment conversations
- Asking: “What do you need right now?”
Above all, know that your child needs you to create a feeling of safety. For example, if a breakdown happens, give them space to feel it all. They may not need your comfort in the moment, but just need to feel. Be ready to comfort them as soon as they ask.
For more honest conversations:
- Use the real diagnosis name when appropriate
- Keep explanations simple and concrete
- Admit when you do not know the answer
- Come back to the conversation again later
- Answer the question your child is asking right now
You might say:
- “The doctors found something going on in your body; we’re learning more.”
- “This has a big name, but we can talk about it one step at a time.”
- “I don’t know the answer to that yet, but I will tell you what I do know.”
- “You can always ask me questions, even if the questions are hard.”
When you approach the difficult questions with honesty, it helps not only your child’s anxiety, but also your own. Being transparent helps children feel trusted and respected, and can ease a parent’s internal stress.
“The honesty also helps when coming out of their parents’ mouths, and they’re talking about it and seeing how their child reacts,” says Christopher. “When you’re trying to minimize something from your child, you’re actually building more anxiety for yourself.”
When feeling overwhelmed, children can borrow calming techniques from the adults around them. But that’s only helpful if you know how to use them. If you’re overwhelmed, hit pause on the conversation. Tell your child that you need a break to do some calming work and ask if they want to join you. Make them part of the journey so they can learn centering techniques and coping skills, too. Try some slow breathing, adjusting your posture, or going for a walk to reset.
Learn more about our free Grief Recovery Method program.

Conversations Around Treatment Time
One of the most helpful ways to make a diagnosis feel less overwhelming is to stay grounded in the present. Children don’t always need the full long-range picture. They often need to know what is happening next.
For medical treatments, they may want to know:
- Who will be with them
- Why is a medication needed
- What the hospital room will be like
- What tomorrow’s appointment will look like
- What part might hurt, feel strange, or feel scary
Christopher encourages parents to break information into small, manageable pieces rather than discussing every possible future outcome at once.
“We don’t know what that moment looks like yet, so we stay in this one,” she says as a type of affirmation anchor to consider.
That approach can calm both the child and the parent. It keeps the conversation from becoming overwhelming.
The Most Common Missteps Parents Make (Out of Love)
When parents are learning how to talk to their child about a medical diagnosis, missteps are often rooted in love, fear, and the instinct to protect. There is no blame here, only awareness. Understanding what can unintentionally increase a child’s anxiety allows parents to approach these conversations with more confidence and care.
Often, children will ask what feel like impossible questions like, “Am I going to die today?” or “Will the doctors make me all better so I can go back to school?”
Here’s a look at a few common missteps (and how to reframe them) for a more open conversation:
Misstep #1: Making Promises You Can’t Keep
In moments of fear, parents often reach for reassurance. Phrases like “Everything will be okay” or promises about future milestones — birthdays, parties, and recovery — can feel comforting in the moment, but they can also create confusion or mistrust if outcomes change.
Reframe instead with phrases such as:
- “We don’t know yet, but we’ll take this step by step.”
- “We’re going to do everything we can.”
These responses offer steadiness without making guarantees that may not be possible to keep.
Misstep #2: Minimizing or Dismissing Feelings
When talking to kids about chronic illness, it’s tempting to try to take fear away. Of course, naturally, you don’t want your child to be terrified of doctors or the medical treatments they’ll be getting. But their fear is real. Statements like “Don’t be scared” or “It’s not that bad” can unintentionally invalidate what a child is already feeling.
Try these phrases instead:
- “Of course you’re scared; this is scary.”
- “This is frustrating. We can sit with it together.”
Naming emotions helps children feel understood and less alone. “Name it to tame it” is a phrase often used in therapy while learning self-regulation skills and labeling emotions appropriately.
Misstep #3: Trying to Fix Instead of Listening
Children don’t always want reassurance; sometimes, they just desire connection. Jumping too quickly into problem-solving can shut down important emotional expressions.
Before jumping in with reassurance, try asking:
- “Do you want me to answer that, or do you want me to just sit with you?”
- “Do you want help, or do you want me to listen?”
- “Do you want to talk now, or later?”
These are small shifts that can help your child feel respected instead of managed.
Letting them take the lead for the conversation can make all the difference in how they open up to you. This can take practice, especially as adults are used to taking charge. Give your child the opportunity to talk instead of grilling them. You might consider sitting with them side by side to lessen the pressure to talk — playing a game on the floor or sitting in the car can offer ideal chatting opportunities.
Above all, invite conversation instead of forcing it.
“We don’t force adults to talk about grief. So why would we force children?” says Clark.
Rather than discussing every possible outcome, break information into small, manageable pieces. Focus on what happens next instead of what may happen months or years down the road. “We don’t know what that moment looks like yet, so we stay in this one,” is a phrase you can use to encourage present-moment thinking.
This approach keeps conversations grounded and less overwhelming.
A Real-Life Parenting Approach
Here are the stories of two of our On Angels’ Wings recipients with children who have had medically-fragile conditions since birth, who have tackled hard questions, medical procedures, and beyond:

Sara and Reiss
For Sara Kaderly, medical conversations started early with her daughter and never really stopped.
Her daughter Reiss, now 13, was diagnosed in utero with a complex group of congenital heart defects now referred to as congenitally corrected transposition.
What was supposed to be a joyful 20-week ultrasound became the beginning of profound grief.
Sara recalls walking into the appointment excited to see her baby and learn the gender, only to leave scared, confused, and unsure of the future.
Looking back, she sees that moment as the start of grieving the unknown, the risk, and the dreams that suddenly felt fragile.
Reiss has since undergone multiple catheter procedures and four open-heart surgeries. Because so much of her early life revolved around adult conversations, hospital stays, and specialty care, Sara says Reiss matured quickly and became advanced verbally.
From the beginning, Sara and her husband chose not to sugarcoat the truth.
“This is her diagnosis, and she needs to be a part of it and understand why,” says Sara.
Teaching the Real Words
Sara believes teaching the actual medical terms helped Reiss feel more included and empowered.
“We didn’t make up words; we talked about the parts of her heart,” says Sara. “If the doctor was in the room and she understood what a valve was, she would know what they were talking about.”
That approach built confidence over time.
Because her parents gave her that control, Reiss learned to ask questions at appointments, speak up, and understand what was happening in her own body. Her parents wanted her to feel “confident enough” to know she has a voice and her voice is important — especially when it comes to medical decisions. “It’s her body and her heart,” explains Sara. “She was asking questions when she was four years old about her heart.”

Giving Reiss a Voice
By the time Reiss faced surgery again at age 10, she was no longer just a toddler being carried through treatment. She understood enough to be scared.
That’s when Sara and her husband leaned into counseling, journaling, giving Reiss space to ask questions, and helping her participate in decisions.
In turn, Reiss started asking a lot of questions whenever she did see a doctor.
Sara says one of the most important lessons for parents looking to navigate conversations with their medically-fragile kid is simply to start. She also strongly encourages counseling before, during, and after major medical moments, especially if the child is open to it. Additional support from child life specialist departments — often a service that is requested by parents — can be extremely helpful for kids navigating procedures, adds Sara.
As of today, her daughter is homeschooled, sings, cooks, and participates in 4-H.
“Outside of her diagnosis, she looks like any other junior high kid you come across,” she says.


Sara adds that connecting with your medically fragile child doesn’t always have to be a boring conversation. She encourages other parents to ask their providers, other parents, and local medical specialty associations for resources. On Angels’ Wings has been a favorite of hers as well over the years.
As for the guilt of being a “perfect” parent, she encourages others to let that notion go.
Perfection, she says, is something that every parent should release when it comes to tough medical conversations. The main goal should always be just to keep children in the loop of what’s going on so they can continue to trust their parents.
“I think that you don’t have to be perfect as a parent. You’re learning just as well as your child is learning,” she says. “I think that it adds trust in the child whenever you have communication with them.”
Caitlin and Bentlee
For Caitlin Smiley, her baby’s diagnosis came not before birth but just after it.

Shortly after her son Bentlee was born, a pulse oxygen reading of 66% confirmed he struggled to breathe. What first seemed respiratory turned out to be a cardiac concern. Within hours, Caitlin learned her newborn had a major heart defect requiring urgent transport and lifesaving intervention.
Just hours after giving birth, Caitlin followed an ambulance to St. Louis to have Bentlee admitted to a pediatric cardiac ICU. Bentlee later underwent open-heart surgery at just five days old, leaving a deep scar down the center of his chest.
“When he first asked me about his scar, I cried,” says Caitlin. “You don’t know how to explain it. I was barely able to process it when they were explaining it to me.”
An interaction with another friend during a swimming outing led to the question that Caitlin will always remember.
A friend pointed at Bentlee’s bare chest and asked, “What happened?”
The child’s parent apologized profusely, and when Bentlee asked about it later, Caitlin explained.
“When you were a baby, your heart was special,” she told him. “Some parts were attached to the wrong side, and the doctors had to help fix that. Your heart just needed a little bit of help. Now it’s strong, and it beats really well.”
Since then, Caitlin and her husband have always tried to keep conversations about Bentlee’s health conditions positive.
“We never wanted to say it was messed up or broken,” she explains.
Now, any time they go for heart echograms, she points out, “Look, there’s your special heart.”
For Bentlee, like many medically-fragile kids, another diagnosis came in 2022 — Common Variable Immune Deficiency, or CVID, a rare primary immunodeficiency that brought repeated illness, infusions, and a whole new layer of medical trauma.
A Lesson on Validation and Medical Anxiety
Bentlee’s immune diagnosis has been harder for him to understand because the treatments are frequent, uncomfortable, and visible in daily life.
Caitlin says that at age 6, much of the emotional “work” is repetition and validation.
When he says he just wants to be a normal kid, they do not brush it off. His parents acknowledge the feeling.
That can sound like:
- “I know this feels unfair.”
- “I know you wish this wasn’t part of your life.”
- “You’re allowed to feel upset.”
Caitlin also learned a tough lesson about how incentivizing medical treatment can backfire.
During Bentlee’s weekly home infusions, which are sometimes part of his CVID treatment, she and her husband tried to pair difficult treatment days with fun things like outings or favorite meals. Their intentions were loving, but Bentlee began to associate “fun surprises” with getting poked.

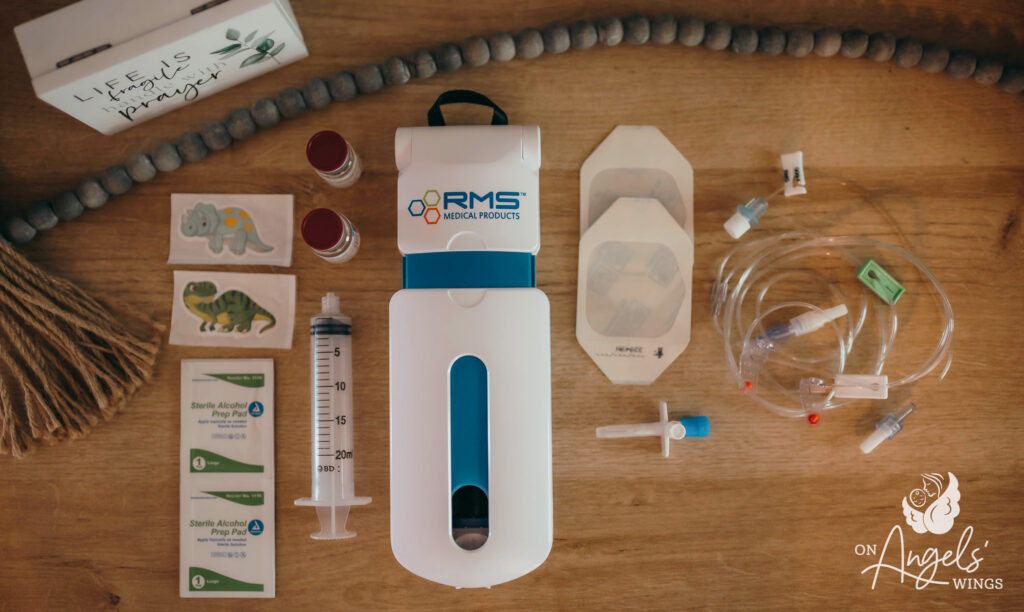
His shots became his “pokeys,” and when they would try to have fun before his at-home injections, fits would ensue.
He started associating with, “Oh, we’re going to the aquarium. Do I have to get my pokey?”
Eventually, even ordinary treats or gifts made him anxious. The breaking point came when he refused to open any gifts at his birthday party because he didn’t want to get shots right after.
“It messed up a lot of everyday things,” Caitlin says of at-home infusions.
Since working with a therapist, they’ve opted to do the shots at the hospital when needed instead. Additionally, giving Bentlee more control has helped him feel a bit more comfortable with medical appointments.
Now, instead of trying to make the day seem perfect, his parents are more direct about what is coming and offer small choices around it.
Sometimes that looks like:
- Telling him about an appointment the day before
- Letting him choose a comforting activity before or after
- Offering a familiar stop on the way to an appointment
That predictability helped rebuild trust.
During that time period, Caitlin admits, “We were facing the guilt; we were the ones poking him, and we tried to make up for it with the best intentions.”
Now, she says, giving him more of a say in the situation helps reduce some of the friction. Counseling helped them understand: “We don’t have to try to make the situation perfect for him.”
Read more of Bentlee’s story here.
When Your Child Resists Appointments or Treatment
Resistance is often fear-based.
When a child melts down about going to the doctor, refuses to get in the car, or fights a treatment, that may be their nervous system saying, “I remember this feeling, and I do not feel safe.”
What can help right away:
- Tell them ahead of time when possible
- Explain the next step clearly
- Validate the fear without backing away from reality
- Offer a small choice where you can
- Keep your tone calm and steady
- Use familiar comfort items or routines
You might say:
- “I know you really don’t want to go.”
- “You’re right; this is hard.”
- “We still have to go, and I’m going to help you through it.”
- “Do you want to bring your stuffed animal or your blanket?”
- “Do you want your special drink before or after?”
It’s important to remember that fear-based guilt isn’t helpful for children to hear. That means avoiding statements like: “If we don’t go, you’re going to get sick and die,” or “if you don’t do this, something terrible will happen.”
Statements like these may create compliance in the moment, but they increase anxiety and erode trust.
Support Exists for Medically-Fragile Families
When you feel like you’re barely treading above water, it’s important to remember your life doesn’t have to be navigated alone.
Luckily, resources exist for families who have special medical needs children.
Sara credits hospital child life specialists as a valuable support in helping Reiss understand and cope with procedures when she was younger. These professionals can explain blood draws, scans, surgery, and hospital experiences in child-friendly ways using pictures, demonstrations, toys, and play.
Child life specialists may offer help by using:
- iPads to show what will happen
- A teddy bear demonstration
- Sensory distraction during procedures
- Simple explanations geared to a child’s age
Other helpful supports may include pediatric counselors, play therapists, school counselors, support groups, faith-based care, peer parents, and service or therapy dogs when accessible.
Caitlin says Bentlee’s service dog, Bear, has been life-changing, especially during anxiety spirals.
“Bear is there for deep pressure therapy,” she explains. “Any time Bentlee starts to panic or go into a spiral of anxiety, Bear will lay across his lap, putting his head on his chest. He will offer his paw. It resets Bentlee’s nervous system.”

Not every family will have access to that type of support, but the principle still matters: children often need practical, sensory, and relational help in addition to words.
Kids’ Grief Program: On Angels’ Wings Legacy of Hope
OAW’s Legacy of Hope Children’s Grief Program is designed to support two underrepresented groups in the children’s grief space: Children who have lost an infant sibling and children living with a terminal-risk diagnosis.
Through Legacy of Hope, OAW aims to fill the often-overlooked gap in care for kids by providing safe emotional outlets, trauma-informed guidance, and access to tools that provide opportunities for healing, expression, and connection.
Legacy of Hope participants can experience a one-day therapeutic camp.
Learn more about Legacy of Hope and how to apply for upcoming camp dates.
Grief Can Be a Part of the Process for Parents
Grief, in all its messiness, is a real part of the equation for medically-fragile families. Parents, especially, are often grieving even if they may not realize it. They’re grieving the life they wanted for their child, the life they wanted for their family, the medical trauma, and the scary things that may be on the horizon.
Clark, who has both professional expertise and personal grief experience, says parents need room to acknowledge that pain.
“Allow yourself to feel the pain and hurt,” he says, noting grief as something our culture often teaches people to avoid or suppress.
“We live in such a grief-phobic society,” he admits.
Avoidance can make things harder. Parents may think being strong means not crying, not naming fear, or holding everything in for the sake of the child. But children notice more than adults realize.
Clark says that when parents hide all emotion, children may conclude that they have to be strong for the adults around them.
So, the question begs: Is it okay to cry in front of your child?
Yes, but with discernment.
It can be healthy for a child to see that sadness is allowed. It helps them understand that tears are not dangerous and that feelings can be named.
You might say:
- “I’m feeling sad right now, and that’s okay.”
- “These are just my feelings. I’m okay.”
- “It’s okay to cry when something is hard.”
At the same time, Clark notes that parents do not need to make their child carry the full weight of adult grief. If you are crying all day or feel emotionally flooded most of the time, it may be time for your own support.
“Grief is so much unlike any other issue,” he says. “It’s the most natural thing we go through. It doesn’t hurt to get yourself or your kid seeing somebody.”

Helping Kids Live Within Limits
Medically fragile children often face painful moments of difference. They may not be able to do all the things their peers can do. They may miss school, sports, parties, sleepovers, or high-exposure activities.
That can trigger grief in children, too.
Caitlin says her family tries not to frame limits as punishments or signs that Bentlee is less capable. Instead, they focus on safety and alternatives.
They might say:
- “You can’t do football, but let’s find something else you can enjoy.”
- “These limits are here to keep you safe.”
That kind of language protects dignity while still honoring reality.
Practical Scripts Parents Can Use Today
When you are under stress, it helps to have a few phrases you may have practiced mentally to prepare for the moment. That way, you can easily work them into a difficult conversation when the time comes for how to talk to your child about a medical diagnosis.
Here are some situational examples and phrases to consider:
When Your Child Asks “What’s Wrong?”
- “Your body has something going on; the doctors are helping us understand it.”
- “You have a condition called ____. We can talk about it one step at a time.”
- “This is part of your story, but it is not all of who you are.”
When Your Child is Scared
- “I know this is scary.”
- “You don’t have to be brave all by yourself.”
- “I’m here with you.”
When Your Child Asks a Question You Can’t Answer
- “I don’t know yet.”
- “That’s a really good question.”
- “When I know more, I will tell you.”
- “We can work together to figure that out.”

When Your Child Resists an Appointment
- “I know you don’t want to go.”
- “You’re right, it’s hard.”
- “We still have to go, and I’m going to help you through it.”
- “I’m right here. You don’t have to do this alone.”
When Your Child Feels Different from Peers
- “It makes sense that this feels unfair.”
- “Your body has different needs, but you are not less important.”
- “We’re going to keep finding ways for you to be you.”
When to Seek Professional Help
Sometimes, the ongoing conversations with your child may not be productive. Additional support for navigating challenging discussions may come from child therapists, family therapists, or spiritual leaders.
Here at On Angels’ Wings, we provide grief recovery services based on The Grief Recovery Method (GRM), providing several certified specialists for one-on-one or group sessions, and it’s free to community members. Caitlin Smiley participated in the program to process her grief surrounding Bentlee’s diagnosis (you can read her story here). This program is for adults only, but parents who participate learn coping skills they can teach to their children.
On Angels’ Wings also offers the Legacy of Hope program, designed in part to help children navigate the grief of a medically fragile diagnosis.
You might consider seeking a professional counselor or therapist for your child if:
- Communication shuts down
- Emotional distress escalates
- Your child asks to talk to someone else
Seeking help is a gift of self-care. It’s also not a failure to ask for support in handling hard-to-navigate conversations. Doing so can alleviate the brain space needed to tackle the other challenging aspects of your child’s medical diagnosis.
Consider seeking additional support for yourself if you:
- Feel overwhelmed most days
- Fear is disrupting daily life
- Crying fits are nonstop
- Emotions feel overwhelming overall
Clark notes that grief is natural, but if most of your day is dominated by crying, anger, fear, or inability to function, it is probably time to get help.
Final Thoughts for Parents Walking This Road
If your child has a life-altering medical diagnosis, you are probably carrying more than most people can see.
You’re likely doing a ton every day that wears on you — managing appointments, medications, insurance calls, school concerns, sibling needs, your own fear, and the ache of loving a medically-fragile child.
And on top of that, you are trying to figure out how to talk about it. Just know: you do not have to do it perfectly to do it well.
If you take anything from this article, we hope that you can:
- Start with honesty
- Answer what you can
- Admit you don’t know it all
- Make room for all the feelings
- Get support when you need it
- Stay with your child in the moment
- Keep conversation opportunities open
As these parents and professionals remind us, kids truly don’t need polished speeches nearly as much as they need safe, truthful connections.
They need to know that what is happening is real, that their feelings are allowed, and that they do not have to face it alone.
Often, that’s where healing begins.

Frequently Asked Questions
Here’s a look at frequently asked questions parents may have about “How do I talk to my child about a medical diagnosis?” that you may find helpful:
How do I talk to my child about a medical diagnosis without scaring them?
Use clear, age-appropriate language and focus on what they need to know right now. Avoid overwhelming detail, but do not hide the truth. Honest, calm communication usually reduces fear more than vague reassurance.
Should I tell my child the actual name of their diagnosis?
In many cases, yes. Teaching the real name can help children feel informed and included in medical discussions. You can pair the medical term with a simpler explanation that they can understand. If the diagnosis name is long or hard to say, work with your child to create a code word or abbreviation that you both can remember and communicate easily. This also helps give the child some sense of control when faced with the unknown.
Is it okay to cry in front of my medically fragile child?
Yes, as long as your emotions are shared in a regulated, age-appropriate way. Seeing a parent feel sad can teach children that emotions are safe. If your distress feels constant or overwhelming, seek professional mental health support for yourself.
What if my child does not want to talk?
Do not force it. Keep the door open, stay available, and offer other ways to process feelings — especially for low-energy days. This may include play, art, books, or counseling. Many children talk when they feel ready and safe. Create safety by also openly sharing some of how you’re feeling. Children mirror adult responses – your honesty will help them be open too.
When should I get professional help for my child or for myself?
Seek support if fear, sadness, or shutdown are affecting daily functioning, school, sleep, family life, or medical care. Counseling, play therapy, grief support, and child life services can all help.